What to Do When You Feel Overwhelmed
The Support and Kindness Podcast: Episode 2
Sometimes overwhelm doesn’t feel like “stress.” It feels like your brain stalls, your chest tightens, your thoughts scatter, and you can’t figure out what to do first.
On Episode 2 of the Support and Kindness podcast, Greg and Rich talk about that exact moment—the one where life gets too loud, too fast, and too much… all at once.
And they start with a truth that matters:

“Feeling overwhelmed doesn’t mean that you’re failing it means that you’re human” — Greg
If you’re here because you’re searching for what to do when you feel overwhelmed, you’re not alone. Let’s turn this into a gentle plan you can use today—especially if overwhelm is connected to ADHD, brain injury (TBI), chronic pain, anxiety, or overstimulation.
Why feeling overwhelmed happens (and why it can feel scary)
Overwhelm is often a pile-up:
- too many inputs (noise, tasks, people, screens)
- too many decisions
- too little recovery (sleep, food, quiet time)
- too much urgency—real or perceived
Rich describes overwhelm in a way many people recognize instantly:

“Slowing down because it’s my brain. It’s because of TBIs. It’s because of ADHD. It’s overstimulation.” — Rich
Overstimulation can flip the nervous system into a freeze response—especially when multiple demands happen at the same time. Rich gives a simple example: phone ringing, an oven alarm going off, and a family member needing to talk—all at once.
In those moments, the goal is not to “power through.”
The goal is to reduce the load—then choose one next step.
Aha! Moment: “Slowing down” is a strategy, not a personality trait
Overwhelm often comes with self-judgment:
- “Why can’t I handle what everyone else handles?”
- “What’s wrong with me?”
- “I should be able to do this.”
But Rich names the real issue: too many inputs + not enough processing space.
And then he offers a practical solution:

“So, I try and slow down. I try and take a moment to just process the things that are making me feel overwhelmed.” — Rich
That’s not avoidance. That’s skill.
And it aligns with mainstream stress guidance: taking short pauses, breathing, and grounding can interrupt spirals and help you regain control of your attention. The CDC explicitly recommends simple actions like deep breathing and taking time to unwind as healthy ways to cope with stress. (CDC)
The 2-minute reset for overwhelm (do this first)
If you feel overwhelmed and anxious, start here. This is the “stop the spin” step.
1) Box breathing for stress and anxiety (1–2 minutes)
Greg shared a tool that’s easy to remember: box breathing.
How it works (4–4–4–4):
- inhale 4
- hold 4
- exhale 4
- hold 4
Repeat for a few rounds.
This matches clinical guidance from Cleveland Clinic on box breathing and how it can help you destress. (Cleveland Clinic)
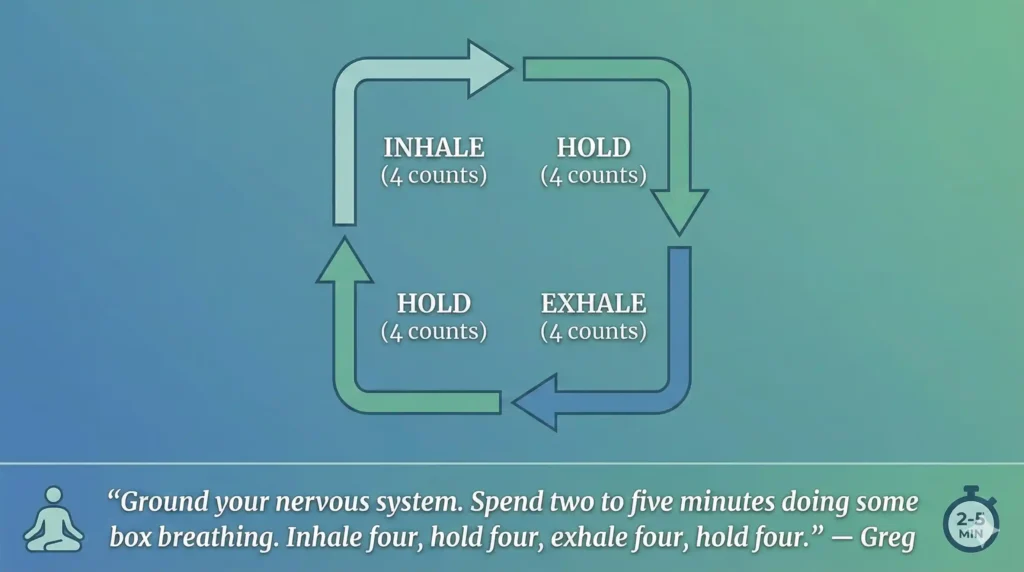
“Ground your nervous system. Spend two to five minutes doing some box breathing. Inhale four, hold four, exhale four, hold four.” — Greg
Try This Today:
Set a timer for 90 seconds. Do slow box breathing. Don’t aim for perfect—aim for slower than before.
2) The 5-4-3-2-1 grounding technique for anxiety (30–90 seconds)
Greg also shares a classic grounding tool:
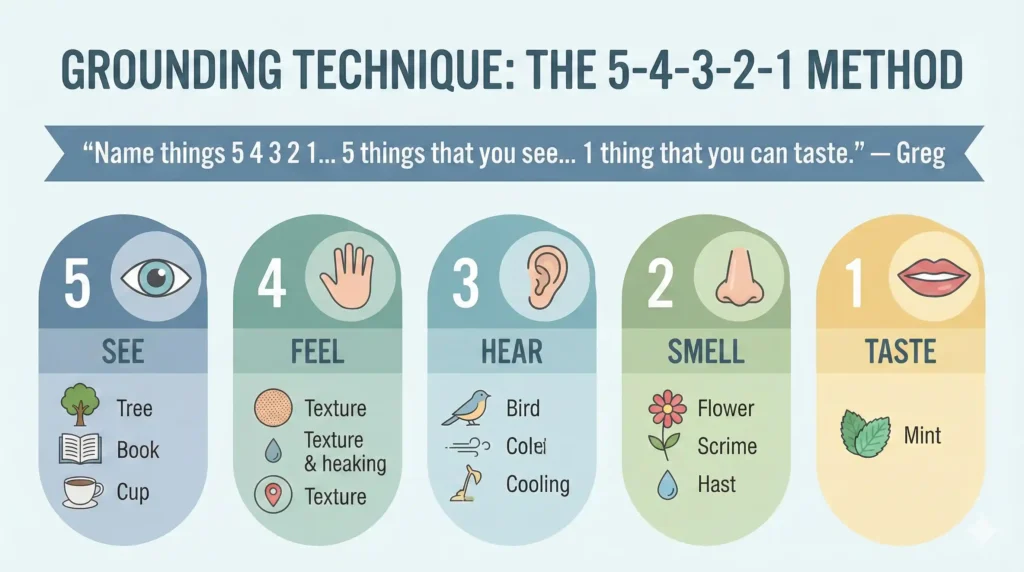
“Name things 5 4 3 2 1… 5 things that you see… 1 thing that you can taste.” — Greg
This technique is widely used to anchor attention in the present moment, including in health-system guidance like the University of Rochester Medical Center’s overview. (University of Rochester Medical Center)
Quick script:
- 5 things you see
- 4 things you feel
- 3 things you hear
- 2 things you smell
- 1 thing you taste
3) Cold water reset (optional, fast)
Greg mentions rinsing hands/face with cool water or holding ice briefly.
This idea shows up in DBT “TIP” skills handouts that use cold temperature to help calm intense emotion quickly. (in.nau.edu)
Common Misconception: “If I can’t calm down instantly, it means it won’t work.”
No—sometimes you’re just moving from a 10/10 to a 7/10. That’s still a win.
Get it out of your head: the brain dump method (3–5 minutes)
Rich and Greg both come back to lists. Because lists reduce mental load.

Rich describes a two-list system:
- a big “looming tasks” list
- a small “today” notepad list
“I also have a notepad on my coffee table of tasks that I need to get done today.” — Rich
Greg adds something relatable (and funny in a painful way): he finds old lists from years ago.
The deeper point is solid: writing it down can be calming because it moves thoughts from “spinning” into “contained.”
Use Greg’s 3-column sort (simple and effective)
Greg shares a structure you can copy:
- Must do today
- Could do this week
- Parking lot (later)
Then:

“circle only one must do item for the next hour and work on that.” — Greg
This is one of the best answers to how to prioritize tasks when overwhelmed: don’t prioritize everything. Choose one next step.
Shrink the next step (when the task feels impossible)
Overwhelm loves big, vague tasks:
- “clean the house”
- “catch up on emails”
- “fix my life”
Greg offers a powerful antidote:

“If the task feels big, cut it in half and then in half again.” — Greg
Examples he gives:
- “write a report” → open doc + first sentence
- “cleaning the kitchen” → clear sink + run dishwasher
- “working out” → put shoes on + 5-minute walk
This is the heart of what to do when you feel overwhelmed at home: pick a tiny step that creates motion.
Overstimulation, ADHD, and brain injury: what to do when your brain freezes
Rich describes a very specific overwhelm pattern:

“when I feel pressured, I freeze up. I completely freeze up…” — Rich
For many people with ADHD, sensory overload can intensify quickly, and CHADD describes how overstimulation can flood attention and coping capacity. (CHADD)
For many people after brain injury, sensory overload can also be intense—BrainLine describes sensory overload experiences and how calming practices like meditation can help some people regain cognitive space. (brainline.org)
A simple “overstimulation plan” you can borrow
If overstimulation is part of your overwhelm (ADHD, TBI, trauma history, chronic pain flares), try this:
- Name the inputs (noise, lights, people, time pressure)
- Reduce one input (mute notifications, step into another room, dim lights)
- Do a 60–90 second reset (box breathing or 5-4-3-2-1) (Cleveland Clinic)
- Choose one priority (what truly must happen next?)
- Communicate clearly (even a single sentence)
Rich highlights how supportive communication can look in real life:

“slow down, dad… It’s alright, take a minute.” — Rich (describing his family)
That’s a model: simple, calm, and non-judgmental.
Ask for help early (it’s a skill, not a weakness)
Greg and Rich both emphasize support systems.
Rich says:

“call on the people around you, to support you, to call on your support system.” — Rich
This is backed by research and major mental health organizations: social support is strongly connected to stress resilience, and the APA explains how support networks help buffer stress. (American Psychological Association)
And peer support is its own powerful category—SAMHSA describes peer support as connection and mutuality between people with shared lived experience. (SAMHSA)
Delegate a piece (not the whole thing)
Greg’s AI-generated list (which he reads on the show) puts it well:

“Ask for help early. Delegate a piece, not the whole project.” — Greg
Try phrases like:
- “I can’t take task A today—can you handle task B?”
- “I need 30 minutes to reset—then I can talk.”
- “Can you summarize these pages for me?”
A surprising example: delegation can build confidence (kids, teams, families)
Greg points out that delegating to children can be empowering—letting them step up and learn capability.
And Rich shares a coaching analogy from soccer: as younger players grow, you can give them more responsibility—eventually they help direct the defense and organize the team.
That’s a great reminder: asking for help isn’t just “taking.” Sometimes it gives other people a way to contribute and feel useful.
Set compassionate boundaries (especially when you feel overwhelmed and anxious)
One of the fastest ways to reduce overwhelm is to reduce commitments—without shame.
Greg reads boundary language directly:

“I don’t have capacity right now. I’ll get back to it tomorrow.” — Greg
Boundaries protect recovery time. And when stress is chronic, health authorities recommend routines that include rest, connection, and caring for the basics. (CDC)
The HALT check: Hungry, Angry, Lonely, Tired
Greg mentions a simple acronym used in recovery spaces:

“don’t get too hungry… don’t get too angry… don’t get too lonely and don’t get too tired.” — Greg
HALT is widely referenced as a self-check tool (including in clinical/public health literature) to catch vulnerability states early. (NCBI)
Use it as a quick diagnostic:
- Hungry: Do I need a snack / protein / water?
- Angry: Am I holding stress in my body or thoughts?
- Lonely: Do I need connection, even small?
- Tired: Do I need rest, reduced tasks, or sleep support?
This doesn’t solve everything—but it prevents you from trying to “think your way out” of a problem that’s really physical depletion.
A gentle “soft landing” routine (end the day without carrying it all)
Greg closes his AI list with a compassionate reminder:

“You do not have to fix everything today. Focus on the next kind step. Small actions count, and they all add up.” — Greg
Try a 3-minute soft landing:
- Write 3 things you did (even tiny wins)
- Write 1–2 priorities for tomorrow
- Do one calming ritual (tea, shower, light reading, breathing)
If you need ideas, the CDC’s wellbeing tips include simple resets like cool water, breathing, and small routines. (CDC)
Key Takeaways (save this section)
- If you’re overwhelmed, start with a 2-minute reset: box breathing or 5-4-3-2-1 grounding. (Cleveland Clinic)
- Do a 3–5 minute brain dump, then sort into today / this week / later.
- Shrink the next step until it’s doable in 2–10 minutes.
- If overstimulation is part of it (ADHD, TBI), reduce inputs first, then choose one priority. (CHADD)
- Ask for help early and delegate a piece—support is protective. (American Psychological Association)
- Run the HALT check to catch depletion before it snowballs. (NCBI)
FAQ (Long-tail keyword phrasing)
1) How to calm down when overwhelmed (fast)?
Start with box breathing (4–4–4–4) for 1–2 minutes, then do a quick grounding pass like 5-4-3-2-1. (Cleveland Clinic)
2) What to do when you feel overwhelmed and anxious at home?
Reduce inputs (silence notifications, close tabs, step into a quieter room), then pick one small next step from a short list.
3) How to stop a panic attack when overwhelmed?
Ground your senses (5-4-3-2-1) and slow the breath. If intense emotion is spiking, some people find cold temperature skills helpful as a rapid “body reset.” (University of Rochester Medical Center)
If panic attacks are frequent or severe, consider professional support.
4) How to prioritize tasks when overwhelmed?
Do a brain dump, then sort into: must do today / could do this week / later—and circle one must-do item for the next hour.
5) How to manage sensory overload with ADHD?
Identify triggers, reduce one input (sound/light/crowds/screen noise), take a sensory break, and use a short reset (breathing/grounding). CHADD discusses sensory overload in ADHD and common coping patterns. (CHADD)
6) How to cope with overstimulation after brain injury?
Plan for breaks, create a calm environment when possible, and use brief calming practices to help your brain “reset.” BrainLine describes sensory overload experiences after brain injury and the value of calming techniques for some people. (brainline.org)
Closing: You don’t have to fix everything today
Greg puts words to what overwhelm can feel like:
“I feel lost and afraid and scared. I don’t know what to do next.” — Greg
If that’s you right now, start with one kind step:
- breathe
- reduce inputs
- write it down
- pick one next thing
- ask for support
And as the show closes:
“Thanks for building a kinder world together.” — Greg
Want peer support?
Greg and Rich share that they host free, confidential, peer-led support groups and invite listeners to visit the website:
“You can visit the website at kindnessrx.org.” — Greg
(Details and times are shared in the episode/show notes.)
Resources Hub
1) Deep Dive Links
- WHO: Doing What Matters in Times of Stress (World Health Organization)
- CDC: Managing Stress (CDC)
- APA: Strengthen Your Support Network (American Psychological Association)
- SAMHSA: General Peer Support (PDF) (SAMHSA)
- ACPA: Ten Steps From Patient to Person (PDF) (ACPA)
2) Media Gallery
Videos
- TED: How to Make Stress Your Friend — Kelly McGonigal (TED Embed)
- TED: All it takes is 10 mindful minutes — Andy Puddicombe (TED)
Podcasts
- APA: Speaking of Psychology — Stress & health (George Slavich) (American Psychological Association)
- The Happiness Lab — Stop Stressing About Stress (pushkin.fm)
3) Action Tools
- Cleveland Clinic: Box Breathing steps (Cleveland Clinic)
- URMC: 5-4-3-2-1 grounding technique (University of Rochester Medical Center)
- TIP Skills (Cold temperature) PDF (in.nau.edu)
- CCI: Worry & Rumination (worksheets + modules) (cci.health.wa.gov.au)
- CDC: Improve emotional well-being (quick resets) (CDC)
4) Citations Used in This Article (clean list)
- Cleveland Clinic (box breathing; grounding techniques) (Cleveland Clinic)
- UR Medicine (5-4-3-2-1 technique) (University of Rochester Medical Center)
- TIP Skills PDF (in.nau.edu)
- APA (social support) (American Psychological Association)
- NCBI Bookshelf (HALT) (NCBI)
- CHADD (sensory overload) (CHADD)
- BrainLine (sensory overload after brain injury) (brainline.org)
- CDC (stress + well-being tips) (CDC)
- WHO stress guide (World Health Organization)
- ACPA Ten Steps PDF (ACPA)
- TED talks + APA podcast + Happiness Lab (TED Embed)